Key Takeaways
-
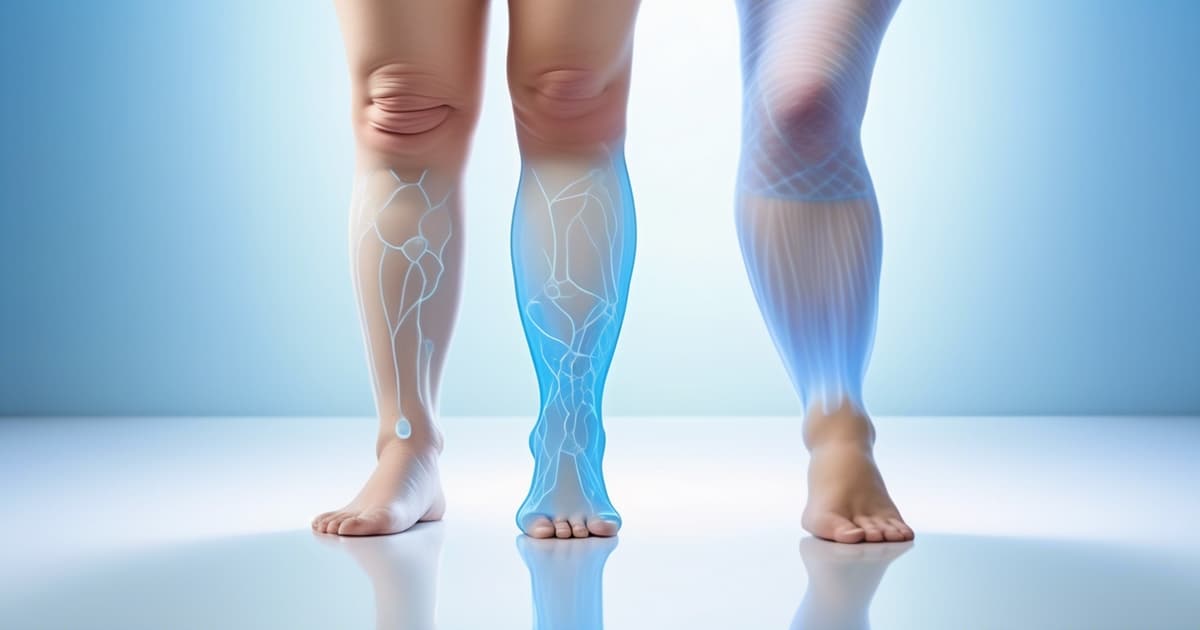
Lymphedema vs lipedema basics Both lymphedema and lipedema are chronic diseases characterized by swelling of the limbs. They have different etiologies, symptomatology, and treatment requirements.
-
Early diagnosis and intervention matter with both conditions to help manage symptoms, reduce complications, and improve quality of life.
-
Lymphedema is lymphatic fluid accumulation due to vessel damage or infection, whereas lipedema is characterized by irregular fat deposits stemming from genetic and hormonal causes.
-
Major differences lie in the parts of the body affected, tissue feel, pain, and sensitivity to calories. This makes proper diagnosis important.
-
Both require personalized management plans that include medical, physical, and sometimes surgical interventions, along with continued follow-up.
-
Mental health, stigma, and patient advocacy are fundamental components of care for patients with lymphedema or lipedema.
Now, lymphedema and lipedema both involve swelling, but they’re not interchangeable.
Lymphedema usually stems from an issue in the lymph system and causes fluid retention primarily in the arms or legs.
Lipedema means that fat accumulates under the skin primarily in the legs and occasionally the arms.
Understanding the fundamentals aids in identifying what distinguishes them and which treatment alternatives are appropriate.
Understanding Lymphedema
Lymphedema is a persistent swelling of the extremities characterized by lymphatic fluid accumulation. It occurs when the lymphatic system, which transports fluid and aids in fighting infection, does not drain fluid effectively. This can cause swelling that becomes increasingly severe throughout the day.
There are two types of lymphedema. Primary lymphedema stems from inherited issues with the lymph system. Secondary lymphedema arises from damage or obstruction, like after cancer therapies or infections. Early detection is important because untreated lymphedema can lead to permanent changes, pain, and additional health issues.
The Cause
-
Primary lymphedema: genetic or inherited changes in lymphatic structure
-
Secondary lymphedema: surgery, radiation, cancer, or injury
-
Infections like cellulitis or filariasis
-
Obesity and lack of movement
-
Chronic venous disease
-
Lymphedema tarda occurs after age 35 because of underdeveloped lymphatic pathways.
When the lymphatic vessels are damaged or obstructed, fluid accumulates in the tissue. It occurs after operation, infection, or even trauma. Infections such as cellulitis can aggravate swelling and harm lymphatic valves.
Lifestyle counts—being less active, carrying some extra pounds, or standing a lot can increase the risk. All of these can impede lymph flow and cause chronic swelling.
The Symptoms
The easiest symptom to observe is swelling, usually in the arms or legs. This edema can begin mild, but typically worsens throughout the day. They can experience a sense of heaviness or tightness.
The skin itself can transform, becoming thick and hard or orange peel-like in appearance, which is a sign called fibrosis. Occasionally, it is painful and can be warm. Skin changes predispose to infection.
Individuals with lymphedema are prone to recurrent skin infections, which may worsen swelling. Initial symptoms can be a sensation of heaviness, tightness in rings or shoes, or diminished range of motion in a joint. Identifying them early can assist individuals seeking proper treatment and prevent the condition from worsening.
The Progression
Lymphedema is a four-staged condition. Stage 0 is no swelling but some lymph system changes. Stage 1 has mild swelling that might subside with elevation. Stage 2 means the swelling does not subside overnight and may involve hardening of the skin.
Stage 3 is severe with thick skin and sometimes large shape changes in the limb. If not treated, the fluid collects and becomes hard. This can lead to fibrosis or lipodermatosclerosis, a hardening of the skin and fat.
Chronic pain and loss of movement are common. Sores or ulcers can occur. The risk for infection increases as swelling and skin changes worsen. Continued management and treatment, such as complete decongestive therapy, compression, and consulting a specialist, assist in decelerating the disease and enhancing life quality.
Compression garments are most effective when applied following manual lymph drainage. Early referral to a lymphedema specialist teaches patients symptom management and reduces the risk of chronic complications.
Understanding Lipedema
Lipedema is a long-term, advancing disease that affects the distribution of fat, primarily in women. It leads to a disproportionate accumulation of fat, primarily in the hips, legs, buttocks, and occasionally arms, but generally not the hands or feet. This causes the limbs to appear disproportionate to the remainder of the body.
Unlike normal obesity, lipedema fat is often recalcitrant to traditional measures such as diet and exercise. Lipedema is frequently misdiagnosed as obesity or lymphedema. Research indicates it has a hereditary component, suggesting that it is genetic. Not every lipedema patient will exhibit all of the symptoms, and this is part of what makes it difficult to identify early on.
The Cause
Lipedema’s root cause is not yet fully known, but genetics are a big piece of the puzzle. A lot of lipedema causes people to have a family member with the condition. Hormonal fluctuations, such as those experienced at puberty, pregnancy or menopause, frequently precipitate or exacerbate the condition. This implicates hormones as a primary factor.
Abnormal fat accumulation is associated with lipodystrophy, in which the body’s fat cells in specific regions become enlarged and more fibrotic. Inflammation in the fat and some lymphatic dysfunction can exacerbate symptoms. These modifications make the fat more painful and less mobile.
Lifestyle factors, including prolonged standing or sitting and inactivity, don’t cause lipedema but can exacerbate swelling or discomfort over time. Unlike obesity, diet doesn’t clear out fat deposits from lipedema.
The Symptoms
Almost all lipedema patients observe bilateral swelling either in both legs or arms that does not subside with rest or elevation. This swelling is unlike lymphedema, which typically involves one extremity and can involve the hands or feet.
The fat in lipedema is painful to the touch and easily bruised since the blood vessels in the fat are fragile. Others experience a feeling of heaviness or tightness. Physical transformations can cause you heartache.
A lot of us are just plain frustrated with others not understanding or with constant misdiagnosis. It is critical to recognize these symptoms early because it allows people to receive appropriate care earlier in the disease process when it can have the biggest impact in slowing the disease’s progression and preserving quality of life.
The Progression
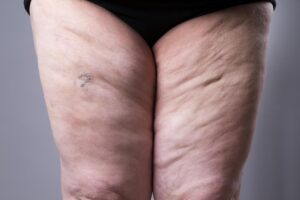
Lipedema has different stages, ranging from minor fat accumulation to significant swelling and fibrosis. Early on, swelling can be mild, but as the disease progresses, mobility may become compromised. A few people get secondary lymphedema, known as lipo-lymphedema, which increases swelling and infection risk.
If untreated, pain and mobility issues frequently increase. Complications such as ulcers, infections, or even alterations to the lymphatic system may occur. Early treatment, whether lifestyle changes, compression, or surgery, can slow lipedema’s progression.
Critical Differences
It’s important to know the critical differences between lymphedema and lipedema to receive the appropriate diagnosis and treatment. They both cause swelling and can feel alike, but they differ in many critical ways from origin and symptoms to their impact on the body.
|
Feature |
Lymphedema |
Lipedema |
|---|---|---|
|
Cause |
Lymphatic damage (surgery, infection, genetics) |
Inflammation, fibrosis, fat tissue changes |
|
Commonly Affected Area |
Limbs, can include hands/feet |
Legs, buttocks, spares feet |
|
Texture |
Firm, fibrotic tissue |
Soft, doughy, nodular fat |
|
Pain |
Rare unless complications |
Often painful, tender |
|
Distribution |
Unilateral or bilateral |
Bilateral, symmetrical |
|
Skin Changes |
Thickened skin, fibrosis |
Nodular, fibrotic fat deposits |
|
Diagnosis |
Clinical exam, medical history |
Exam, ultrasound, MRI |
|
Prevalence |
All genders |
Mostly women |
|
Triggers |
Surgery, infection, trauma, genetics |
Hormones, trauma, lifestyle |
1. Body Location
Lymphedema typically impacts either one or both arms or legs, though it can present in other parts of the body, such as the face, chest, or trunk. It occasionally involves the hands and feet, distinguishing it from lipedema.
Lipedema primarily strikes the lower body, specifically the thighs, hips, and buttocks, while sparing the feet. This almost invariably presents bilaterally in a symmetrical fashion.
Swelling in lymphedema could begin in a single limb after cancer surgery or infection. Lipedema typically begins in the hips and extends downwards, terminating at the ankles, with a distinct “cuff” at the ankles where swelling ceases. Recognizing these patterns assists patients and providers alike in nailing the right diagnosis.
2. Tissue Texture
Lymphedema’s swelling is hard, dense and often fibrotic. That causes the tissue to harden over time, sometimes resulting in areas of thick skin or ‘hard patches’.
Lipedema patients sense a soft, doughy, or sometimes lumpy sensation beneath their skin, with nodules in the fat. This softer aspect is typically more crushable.
These texture distinctions are helpful in clinic exams and can steer you toward the appropriate therapy. Lymphedema may require therapies for fibrotic tissue, whereas softer lipedema may be better suited to massage or compression.
3. Pain Presence
Lipedema is characterized by pain, tenderness, and easy bruising in the affected areas. The pain is relentless and often excruciating, impairing mobility and everyday activities.
Lymphedema is typically painless unless infection develops or skin becomes very tight. This implies lymphedema patients might not feel any pain until the issue becomes serious.
Lipedema pain frequently requires additional pain control and assistance.
4. Foot Involvement
Swelling from lymphedema frequently shifts into the feet and ankles. This can lead to issues with footwear, movement, and skin.
Lipedema stops at the ankles, rarely affecting the feet. This obvious boundary is the primary hint that distinguishes the two.
Feet that change due to lymphedema could translate into shoe changes, skin checks, or added care to prevent wounds.
5. Response to Diet
Diet changes alone don’t always help lymphedema. The swelling is tied to lymph fluid, not fat, so even with weight loss, swelling can remain.
Lipedema patients often find it very difficult to lose weight as lipedema fat is resistant to diet or exercise in comparison.
Both groups may benefit from customized nutritional programs to optimize health. However, fat loss expectations need to be tempered. Nutrition can aid with inflammation and overall wellness.
The Diagnostic Path
Diagnosing lymphedema and lipedema calls for a careful, multi-step process. These two conditions share some signs, like swelling, but each one has its own patterns and causes. A full evaluation looks at symptoms, medical history, and family history to pinpoint the root of swelling and stop the problem from getting worse.
Since treatments for lymphedema and lipedema differ, knowing which one is present is key for effective care.
Clinical Evaluation
A comprehensive clinical diagnosis begins with an intimate examination of symptoms. Unilateral swelling, heaviness or tightness of extremities, pain and skin alterations can suggest lymphedema. Lipedema, by comparison, typically exhibits symmetrical swelling in both legs with the feet being spared and is tender to touch.
The next step is a full medical and family history. Previous surgeries, cancer treatments, infections or relatives with the same issues can all be relevant. Physical exam assists in figuring out the stage. For lymphedema, they check for pitting, which is denting after pressing the skin, skin texture, or body contour changes.
For lipedema, the doctor tests for a soft, rubbery texture, easy bruising, and non-responsiveness to diet or exercise. Eliminating alternative causes, such as obesity, lipodystrophy, or cardiac and renal issues, is a significant component of this phase.
A comprehensive strategy must be used, since there is no one test that can diagnose these conditions by itself. It is that physician’s seasoned judgment, armed with all of the facts, that helps steer the right diagnosis and next steps.
Imaging Techniques
-
Lymphoscintigraphy: This test uses a small amount of radioactive dye injected under the skin. It lets doctors watch the flow of lymph fluid and detect any blockage or leakage. It is the gold standard for demonstrating lymphatic function.
-
Ultrasound: Often used to rule out blood clots or check for fluid collections. It can discern fat from fluid.
-
Magnetic Resonance Imaging (MRI): Helpful for seeing the structure of soft tissues. MRI can detect changes in lymphatic vessels or identify fat accumulation in lipedema.
Lymphoscintigraphy is best at demonstrating lymphatic obstruction. By tracing the flow, it aids in verifying lymphedema in ambiguous cases. Imaging directs therapy by indicating the extent of the limb and the location of the pathology.
It provides a fuller picture, allowing physicians to design treatment around actual information. High quality imaging counts. It aids in confirming the diagnosis and allows care teams to quantify the stage and severity of the disease.
That way, the treatments selected fit each individual’s needs.
Management Approaches
Lymphedema and lipedema require specialized treatment. Each condition responds best to a combination of approaches tailored to the individual’s needs and symptoms. Care typically combines physical therapy, lifestyle modifications, and occasionally surgery to control the swelling, discomfort, and tissue changes.
Lymphedema Care
A good lymphedema plan will incorporate complete decongestive therapy to shrink limb size and soften the hardened tissue. This includes manual lymph drainage, compression wraps, skin care, and exercise. Compression therapy may reduce the risk of recurrent cellulitis, so medical grade garments are essential. Evening folks might require short-stretch wraps or pneumatic compression pumps to receive the highest advantage.
Manual lymph drainage is a type of massage that pushes lymph fluid out of swollen areas. When utilized as a component of full decongestive therapy, it helps prevent fluid from accumulating.
For the unlucky who don’t get sufficient relief with conservative measures, typically a 5% to 10% volume decrease, surgery can assist. Lymphaticovenular anastomosis establishes new drainage routes, with vascularized lymph node transfer or debulking surgery being a possibility for more pronounced cases.
Education and self-care do factor in. Individuals with lymphedema must learn how to recognize infection, properly care for their skin, and utilize their garments and devices appropriately. Daily support from a clinic or support group keeps people on track.
Check-ups with health care teams allow plans to adjust as symptoms move. Keeping in touch with your providers helps you catch problems early and keeps care up to date.
Lipedema Care
Management for lipedema begins with compression garments that provide constant pressure and alleviate pain and swelling. We wear them all day. Intermittent pneumatic pumps can provide assistance to some, as well as exercise and a healthy diet.
Bariatric surgery can be an option for individuals with a BMI greater than or equal to 40 kg/m², or greater than or equal to 35 kg/m² in the presence of complications, when other methods of weight loss have failed.
Liposuction, which is frequently the key surgical component, eliminates the fibrotic fat that accumulates. Lipedema reduction surgery can relieve pain and facilitate movement. Noninvasive treatments such as extracorporeal shockwave therapy may assist by stimulating new blood vessel formation and tissue regeneration.
Care should be a multidisciplinary team effort. Doctors, therapists, nutritionists, and even surgeons are involved at times. This team approach addresses physical, emotional, and lifestyle needs.
It’s education so folks know what treatment options are out there and how easy adjustments, like low-salt diets or water aerobics, can make a difference. They need a support network, both to live well with lipedema and to make sense of the options open to them.
Beyond The Physical
Lymphedema and lipedema are about much more than what’s on the skin. Both drive daily battles that extend into emotional wellbeing, relationships, and self-perception. The effect is usually unseen, but it defines the way we all live and survive.
Emotional Toll
Chronic swelling and pain from these conditions can erode mental fortitude after a while. It’s a cycle of frustration and worry, many patients report. Little things such as walking or standing become difficult and this can make you feel powerless or even frustrated.
Nights can be rough, with deep aches and pains in the arms or legs that keep people up. As time passes, this sleep deprivation makes it more difficult to control stress and mood. Affectations of body shape due to swelling or excess fat accumulation can impact self-esteem.
Some skip mirrors or dinners with friends because they feel judged. They could overhear careless remarks about their stature or receive guidance that overlooks their health requirements. This can result in seclusion, with individuals retreating from loved ones.
The fear of being misunderstood compounds anxiety and can make social situations feel suffocating. Support for mental health is essential. Speaking with a counselor or participating in a therapy group can assist individuals in acquiring coping mechanisms.
Peer groups, in person or online, provide a secure forum to exchange narratives and advice. These communities can disrupt the loneliness spiral and demonstrate that others understand the same battles.
Social Misconceptions
A lot of people still believe these are purely “weight” issues or “appearance” issues. This pervasive myth is dangerous because it can postpone diagnosis and appropriate treatment. People with lymphedema or lipedema often hear advice to “just eat less” or are told the swelling is their fault.
This stigma can prevent individuals from pursuing assistance or cause them to question the legitimacy of their ailment. We need public education to alter these perspectives. Awareness campaigns help demonstrate that both are legitimate medical issues rather than cosmetic.
Advocacy groups deploy narrative, statistics, and engagement as countermeasures to misinformation. The more people know, the less inclined they are to judge or perpetuate myths. Advocacy is not only for patients. Friends, family, and healthcare workers can all play a role in speaking up and sharing facts.
Such collaboration can help make society more inclusive and affirming.
Patient Advocacy
Patient advocacy fuels authentic makings of care and public awareness. Lymphedema and lipedema groups assist patients in obtaining essential supplies, discovering empathetic physicians, and advocating for innovative research.
By becoming members of these organizations, individuals can educate themselves regarding their rights and receive information on emerging treatments. Even without a circle, patients can advocate at clinics. Small gestures, such as asking questions, taking notes, and bringing a support person to appointments, can have a huge impact.
When patients tell us their stories, they can help other patients not feel so alone and help health workers understand what is important. Collaboration between patients and doctors produces the best results.
Open conversations on symptoms, side effects, and day-to-day difficulties establish trust. This type of care considers the entire individual, not just the inflammation or discomfort.
Conclusion
Lymphedema vs lipedema basics Lymphedema and lipedema often look alike at first. They both have their own different signs, causes, and needs. Understanding these basics aids in identifying the correct diagnosis and selecting the most effective course of treatment. Physicians treat each with different tests and different checks, so the right plan is crucial. Good care extends beyond the body. It boosts spirits and facilitates living. People anywhere in the world deal with these problems. Getting to the truth early can prevent things from escalating. For healthier lives, know more, ask questions, and chat with knowledgeable health teams about these conditions. Share your story or read more trusted info to help others get answers as well.
Frequently Asked Questions
What is the main difference between lymphedema and lipedema?
Lymphedema is swelling that occurs from lymph fluid buildup, typically in an arm or leg. Lipedema is a stubborn fat condition, primarily in the legs and occasionally the arms, but it never affects the hands or feet.
Can lymphedema and lipedema occur together?
Yeah, they are both possible to have together. Lipo-Lymphedema is when people with lipedema can develop lymphedema.
How is lymphedema diagnosed?
Lymphedema is diagnosed through a physical exam, medical history, and sometimes imaging tests like ultrasound or MRI to check lymphatic function.
How is lipedema diagnosed?
Lipedema is typically diagnosed by a healthcare provider through symptoms, physical examination, and excluding other causes of swelling or fat accumulation.
Are there cures for lymphedema or lipedema?
There are no cures for either. Treatments aim to relieve symptoms, decrease swelling, and enhance quality of life.
What are common management options for both conditions?
Both can be supported by compression, manual lymphatic drainage, gentle exercise, and a healthy diet. Surgery is considered.
Is early treatment important for lymphedema and lipedema?
Yes, early treatment controls symptoms, prevents complications and makes you feel better as a person. Timely management can reduce advancement and improve quality of life.